CAPE FEAR REGION — New Hanover Regional Medical Center (NHRMC) and other regional hospitals face a possible shortfall of beds, ventilators, and personal protective equipment that would be needed to respond to a potential spike in Covid-19 cases in the coming weeks.
Models for the potential increase in Covid-19 cases show that the demand could be several times the region’s total capacity — but a major factor is timing. Thousands of cases could still be handled if they are spread out over a long enough period of time. But a sudden surge in cases could create the need for thousands of hospital beds and ventilators, a situation currently unfolding in New York City.
NHRMC has 769 licensed beds, about 100 ventilators, and “adequate supplies” of face masks and other personal protective equipment (PPE) to protect staff and health providers at this time, according to NHRMC spokesperson Julian March. He said the hospital began accepting PPE donations from the community last Monday.
“We are working with our suppliers to secure more for the future,” March said.
On Monday the hospital announced it had set up a 2,100-square-foot tent hospital next to the 17th Street Emergency Department to give staff more space to care for patients during the pandemic. It will also limit exposure to “potentially infectious diseases and accommodate additional demand for [its] services,” according to James Bryant, Administrator of Emergency Services.
‘Today, our ventilator supply meets our needs’
On March 23, the state recommended that patients with mild Covid-19 symptoms do not need testing and should recover at home and call their doctor. March said this guidance allowed NHRMC to preserve PPE and other resources to care for those with more severe symptoms.
Additionally, he said the hospital is talking with other providers to bring in more ventilators or “coordinate how to get patients to that level of care.”
The state had issued temporary authority to exceed capacity limits to enable hospitals to respond to the pandemic, according to March.
“We have also cancelled or postponed surgeries that can wait to have more beds available when we need them,” March said.
To protect patients, staff, and providers from exposure, March said the NHRMC has isolation rooms and are working to create additional negative pressure rooms — rooms that allow air to flow in but not out to prevent contamination between rooms. If needed, he said the hospital also has the ability to designate larger areas for isolated patients.
In Southport, Dosher Hospital has 25 beds and two ventilators, but as a “community critical access hospital” it does not have an intensive care unit and would transfer Covid-19 patients experiencing respiratory issues to other providers.
“So if this area gets hit hard, God forbid, we would send a lot of patients out to other facilities that have intensive care units, or have a tertiary level of care where they have specialists on staff, such as pulmonologists, whereas we don’t have those specialists on staff,” Dosher spokesperson Ilene Evans said.
As a critical access hospital without an ICU, she said the two ventilators have “always been commensurate to the type of care we provide.”
Last Friday, Dosher announced it was also accepting PPE donations, including surgical masks, N95 face masks, and surgical gloves. It said it would also receive donations for homemade hand-sewn cloth masks, although such masks wouldn’t be used unless all other supplies are exhausted.
“Our supplies are adequate, however, it is anticipated that our need for PPEs will elevate, commensurate with the recorded number of COVID cases in our area,” according to the release.
A spokesperson for Novant Health, which runs the Brunswick Novant Medical Center in Bolivia, said the hospital currently has 74 beds, although the total number can fluctuate “by the hour.”
“The state of North Carolina lifted a restriction last week that will allow us to open more beds if needed,” the spokesperson, Kristen Barnhardt, said. “We can temporarily add and relocate beds into any space that meets federal safety requirements if we have a surge.”
Novant routinely monitors and diversifies its supply chain, according to Barnhardt, while its emerging infectious disease team is monitoring the situation closely.
“Today, our ventilator supply meets our needs,” Barnhardt said last Monday. “Since it is simply unknown if we will have a surge of patients at once, we are working to increase the amount of ventilators we have on-hand should we need them.”
Another spokesperson, Megan Rivers, said Novant Health is bracing for shortages of PPE and other supplies.
“If you turn on any news station, you will see this concern is not unique to Novant Health’s team members. We share these valid concerns and frustrations,” Rivers said. “Yet, as of today, Novant Health is not experiencing a shortage.”
She said there will likely be more shortages in the near future, as there will be for hospitals across the country.
“By knowing how and when to appropriately use PPE, our hope is that team members will be able to safely care for patients while extending the life of supplies during this critical time. However, we know this is only one solution and it simply does not suffice,” Rivers said.
Novant will continue to try and solve PPE challenges as part of the larger U.S. supply chain shortage, she said, while calling on the government to “work expeditiously on solutions to help all healthcare systems secure the resources we need to protect our team members and patients.”
On Monday, Governor Roy Cooper signed an executive order that frees up the state’s surplus supply of PPE for “frontline healthcare workers.”
Possible shortages
On Sunday, New Hanover County public health officials announced they were investigating two new positive cases of Covid-19, both of which “appear to be community transmission and are not travel related,” bringing the county’s total number of positive cases to 27 as of the end of the weekend. Three more cases were identified on Monday, bringing the total to 30. The first ‘presumptive positive’ case was identified on March 18, less than two weeks earlier, while the first case of community transmission was announced on March 24.
Brunswick County said it had confirmed 14 positive cases and were waiting for 301 test results as of Monday. Last Friday, Pender County spokesperson Tammy Proctor said the county does not yet have a positive coronavirus test.
As of Monday, North Carolina had confirmed 1,307 cases across the state, an increase of 140 from Sunday’s numbers.
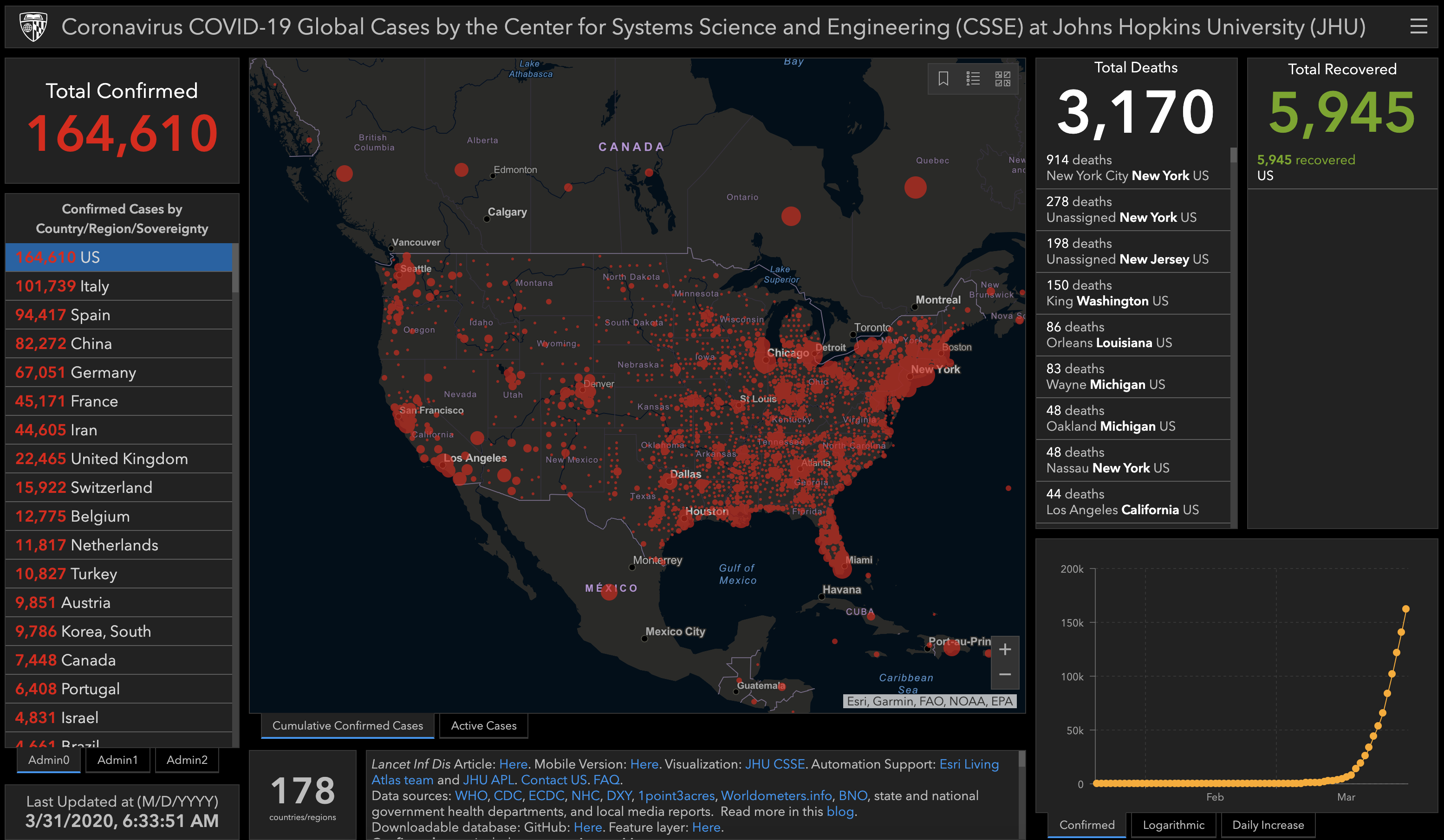
Meanwhile, the number of Covid-19 cases and deaths nationwide continue to exponentially increase. While the U.S. passed 160,000 confirmed cases Tuesday morning, according to numbers compiled by John Hopkins University, deaths caused by the novel coronavirus have tripled since Thursday, when they totaled just over 1,000 — that number has now reached 3,170. More than 900 U.S. deaths have been reported in New York City alone.
On Sunday evening, Dr. Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases, told CNN that 100,000 to 200,000 Americans could potentially die from Covid-19. He also acknowledged the projection, based on current models, is a “moving target.” A few hours later, President Trump extended public coronavirus restrictions through April, citing Fauci’s estimates.
On March 26, the Center for Disease Control and Prevention (CDC) said the U.S. is now “in the acceleration phase of the pandemic,” with more than half the country seeing some level of community spread of Covid-19.
“CDC expects that widespread transmission of COVID-19 in the United States will occur. In the coming months, most of the U.S. population will be exposed to this virus,” according to a CDC situation summary.
It warned that public health systems may become overloaded, “with elevated rates of hospitalizations and deaths” while healthcare providers and hospitals “may be overwhelmed.”
Officials at the CDC conferred with worldwide epidemic experts in February, according to the New York Times, creating four different models that predict between 160 million and 214 million Americans could be infected over the course of the pandemic.
On the conservative end, this represents 48.4% of the U.S. population (according to current U.S. Census Bureau’s population estimate of 329,454,295). At the high end, this represents 64.8% of the population. The CDC’s scenarios also suggested that 2.4 million to 21 million Americans could require hospitalization (between 0.73% of the population and 6.37% of the population).
According to 2017 U.S. Census estimates, the population of New Hanover, Brunswick, and Pender counties totaled 440,353 (NHRMC also provides services in Columbus, Bladen, Duplin, and Onslow counties). Assuming .73% of the three-county region’s population would require hospitalization over the course of the pandemic, the region’s hospitals would require a total of about 3,000 beds (according to 2019 U.S. Census Bureau population estimates). Assuming 6.37% of the population would require hospitalization — CDC’s worse-case scenario out of the four separate models — about 27,700 beds would be required.
The amount of total beds provided by the region’s hospitals — NHRMC (769), BNMC (74), and Dosher Hospital (25) — is 868.
Data on how many patients will require ventilators is still limited. Early data from China showed 12% of Covid-19 patients required some form of ventilator to breathe, but more recent data shows only around 1% of patients needed breathing assistance, according to STAT (a healthcare news outlet produced by Boston Globe Media). Based on this, if half the regional population were to contract Covid-19, about 2,000 would ultimately require ventilation at a hospital or medical facility.
Some of these models show that the region’s resources of hospital beds and ventilators could be outstripped, by an order of magnitude, by the demand created by a surge in Covid-19 cases. However, it’s important to note that even models with ‘sharp peaks’ — those that see many cases at the same time — don’t involve everyone getting sick at the exact same time. The amount of time over which the total number of cases is spread is, for many public health officials, the key variable.
Send tips and comments to [email protected], @markdarrough on Twitter, or (970) 413-3815